Electronic Prior Authorization Reform: What’s Next?

ACMA
Aug 17, 2022
6 minutes read

On July 27, 2022, the Seniors’ Timely Access to Care Act of 2022 (H.R.3173) moved one step closer to becoming a law. Initially introduced in 2021, the bill received modifications this week, and the House will vote on the legislation in the Fall of 2022.
The legislation will create electronic prior authorization (ePA) guidelines for Medicare Advantage plans under title XVIII of the Social Security Act. ePA is the electronic process of submitting PAs, allowing real-time medication approval.
The legislation will streamline the prior authorization process for the more than 28 million Medicare Advantage members. Medicare Advantage (MA) plans, sometimes called “Part C” or “MA Plans,” are Medicare-approved plans from private companies offering an alternative to original Medicare for health and medication coverage.
Similar to other private insurance plans, MA’s prior authorization (PA or prior auth) processes have placed an unnecessary burden on providers and created barriers for patients to receive timely care. PAs require providers to receive approval for coverage (i.e., payment) for certain medications and medical services from insurance companies or payers. Typically, prior auths are submitted through phone or fax.
However, ePAs are becoming more popular as they increase patients’ ability to receive timely care. Electronic PA requests result in 40% more same-day determinations than manual PAs. HCPs can spend 14.9 hours a week on traditional PAs, but ePAs can significantly reduce this time.
The Senior’s Timely Acess to Care Act represents progress towards uniform ePA guidelines and will significantly improve the patient-doctor relationship. Understanding ePAs and their benefits will help anyone see how the legislation will benefit patients and providers.
Electronic Prior Authorizations: Basics
What are Electronic Prior Authorizations?
Electronic prior authorizations (ePAs) refer to the electronic process HCPs use to communicate with an insurance company to receive approval for medications or services. The National Council for Prescription Drug Programs (NCPDP), the leading non-profit pharmacy standards development organization, created ePA standards, and many states have already adopted these standards. However, at the national level, the Seniors Timely Access to Care Act is one of the first steps towards a national ePA standard.
The NCPDP’s SCRIPT Standard, a standardized e-prescribing system, offers a standardized ePA form, facilitating the exchange of information between the prescriber and payer. The standardized ePA will further reduce the time required for providers to complete the PA process and help providers accomplish the following:
- Determine whether a PA is necessary for a particular service or medication
- Respond promptly and efficiently to payer requests for additional information.
What are the Benefits of Electronic Prior Authorizations?
Overall, the benefits of ePAs include:
- Reducing burden
- Increasing efficiency
- Improving care
- Decreasing redundancy
- Reducing manual effort.
The Advancing Health Insurance Providers (AHIP) group created the Fast Prior Authorization Technology Highway (Fast PATH) initiative to understand the impact of ePAs better.
Using data collected from over 40,000 prior authorizations, the Fast PATH initiative analyzed data on PA trends before and after the implementation of ePAs. The results of their findings are summarized and illustrated below.
Figure 1: AHIP Fast PATH report found after implementing ePAs, patients received care faster, providers received payer decisions quicker, and providers better understood the PA process.

The results of the AHIP Fast PATH report revealed that ePAs impact patient care in the following ways:
- Enhancing Speed of Care:71% of providers reported patients received care faster after implementing ePA.
- Reducing Waiting Time:ePA requests were submitted three times faster, resulting in a 69% reduction in the average waiting time between submission and decision from the health plan.
- Easing Provider Burdens from Phone Calls and Faxes:ePAs reduced phone calls by 54% and faxes by 58% among providers.
- Providing Better Information to Providers:60% of experienced users said that ePAs made the PA process easier to understand.
Ultimately, providers must be trained, workflow integration needs to be implemented, and incentives should be established to encourage providers to use ePAs.
When Are Electronic Prior Authorizations Not Used By Providers?
As a result of the significant benefits of ePAs, the use of ePA is embraced by healthcare networks across the board, with almost 100% of pharmacies and payers adopting the technology. Although ePAs have been progressively integrated over the past decade and have confirmed benefits, approximately 50% of PA requests are still sent via phone or fax.
Many providers still use phone or fax for PAs in the following situations:
- 33% prefer phone or fax to ePA when completing urgent requests.
- 28% of prescribers use non-electronic methods when handling complex prescriptions.
- 80% of users use non-electronic methods when unsure whether ePA is available.
- 19% of specialty medications are submitted manually.
PAs submitted electronically are typically determined within two hours, with 43% being determined automatically. Provider confusion and the lack of standardization have created an obstacle to the comprehensive integration of ePAs across the U.S. healthcare system. Additionally, the lack of uniform PA policies complicates the adoption of ePAs.
State Electronic Prior Authorization Reform
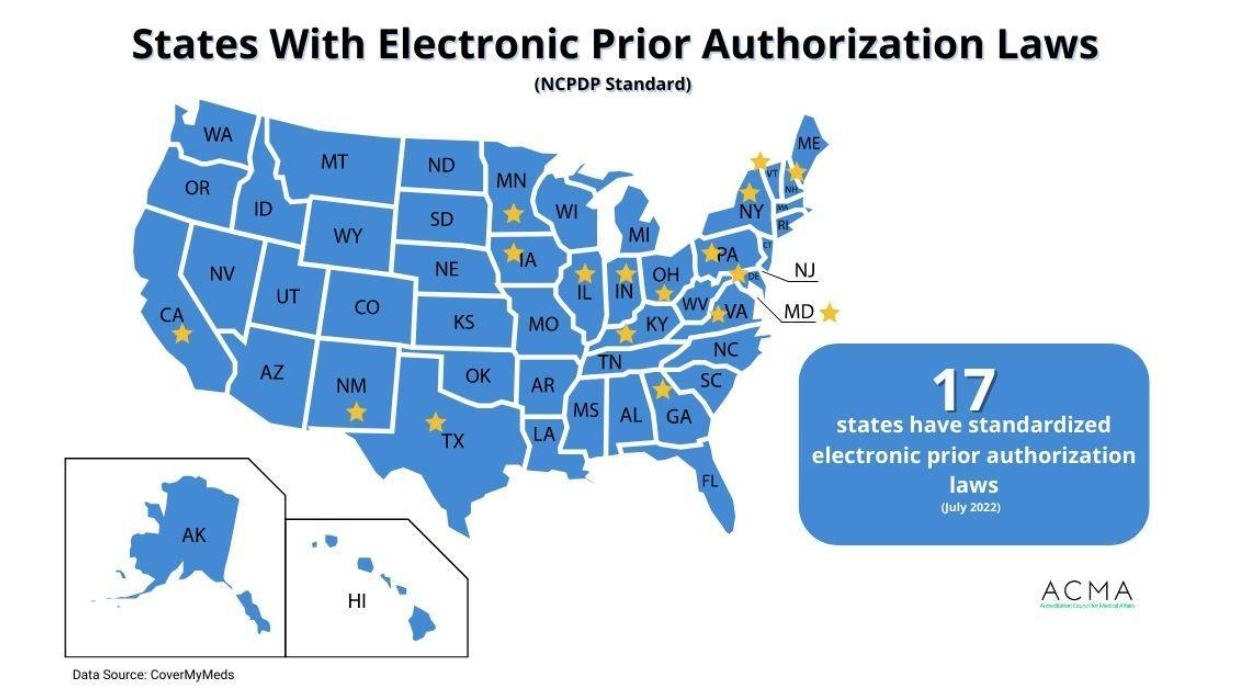
Only a few states have passed ePA laws as of August 2022, and even within those states, there are varying degrees of standardization. The laws vary from requiring standardized forms to using the NCPDP SCRIPT Standard forms. Figure 2 reveals the 17 states with laws requiring the use of the NCPDP’s SCRIPT standard.
Figure 2: States using the NCPDP’s SCRIPT Standard for ePAs
The Future of Electronic Prior Authorization Reform
Increasing ePA use will require government intervention at the federal level. The Seniors’ Timely Access to Care Act represents progress toward the uniform adoption of ePAs across the US. Medical associations have unanimously supported the Seniors’ Timely Acess to Care Act and applauded the bill’s movement, including the American Medical Association (AMA), saying the following this week:
“On behalf of the physician and medical student members of the American Medical Association (AMA), I write in strong support of the “Improving Seniors’ Timely Access to Care Act of 2022,” as amended by the Ways and Means Committee. The legislation, as originally introduced, garnered more than 300 bipartisan House cosponsors and the support of approximately 500 physician, hospital, patient, and insurer organizations. We greatly appreciate the Ways and Means Committee for scheduling a legislative markup and strongly urge swift passage of this bipartisan bill that will help streamline, simplify, and standardize prior authorization processes within Medicare Advantage (MA) plans.”
The next step for electronic prior authorization reform is passing the legislation in the Fall of 2022. More than 28 million MA members will benefit from this bill, improving healthcare quality and reducing waiting times for medication.
To learn more about prior authorizations, read the Evolution of Prior Authorizations. To learn about the benefits of certifying your team as certified prior authorization specialists, read about the benefits of certification.
